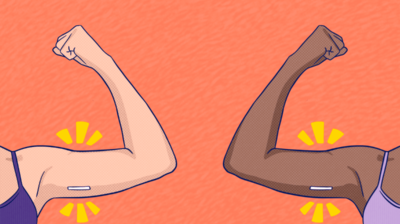How I found the right contraception for me
Izzy outlines her journey switching from the pill to the implant and how we all deserve more when it comes to sexual health.
Casting my mind back to my secondary school sex education experience, I find very little of note to discuss. I recall an intensely awkward, stand-alone class in which one teacher – who we students all regarded as a kindly, grandmother type – proceeded to explain how to fix a condom on an erect penis.
I recall vague discussions of the pill and the necessity of taking it every day; I remember some classmates were desperately concerned with the potential “weight gain” side-effect associated with the pill, which my form teacher roundly shut down with “the side-effect of unprotected sex is a baby”.
Perhaps as a consequence of my secondary education across the border in the North, my cohort was lucky enough to experience a two-part presentation on consent. In a time when “stop raping me” was still playfully giggled out in response to flirtatious tickling, I feel that our little old Catholic school was really ahead of the curve on this issue.
These presentations, delivered by an external body, hammered home the message that sexual consent is not the absence of a verbal “no”, it is an enthusiastic and all-encompassing “YES”. When I later started third level, I was disappointed, but unsurprised, to find that many of my new college friends had had no such consent education prior to a Freshers Week workshop on the subject.
Room for improvement
Although sex education as a concept is gaining traction in secondary schools, there is still a great deal of room for improvement. Consent aside, my less-than-satisfactory sex ed. informed me on two points:
It’s really not that outrageous for me to say that I learned much more about sexual health through personal experience and research than I ever did from school.
At the age of 16, I became what most GPs heteronormatively describe as “sexually active” (involving penetrative, penis-in-vagina sex). I quickly became accustomed to the use and application of male condoms. What I remained ignorant of for too long was lubricant. As you might imagine, lube just helps the whole process go more smoothly, and consequently, more pleasurably.
Whilst I had a lot of fun in my earliest days of sexual activity, I berate myself profusely for not using lubricant from the start (though in fairness, lube appeared nowhere on my school’s two-point list of sex necessities). Although finding the right lube can be reminiscent of Goldilocks and the Three Bears (“this one dries too quickly, this one is too sticky, this one is just right!”), it was a trial-and-error process that I found well worth the investment.
Having become “sexually active”, I was put on the pill. I didn’t question my GP when she prescribed me the pill, and she did not elaborate on the many other contraceptive options available for young people like me, or even on the other versions of the pill that existed.
It didn’t occur to me to wonder if my prescription was progestogen-only or combined, I just took the damn thing once a day for several months before I decided I didn’t want to be tied down to a daily prescription so early in my life.
Figuring out what contraception suited me
It wasn’t until college, when I engaged in many long, detailed conversations about contraception, that I realised there was no one pill; there were different kinds! For different bodies! For different needs and requirements! More than that, I learned about the complexities of taking birth control pills as a means of managing endometriosis and polycystic ovary syndrome – conditions that had never passed through the lips of teachers during my limited sex education.
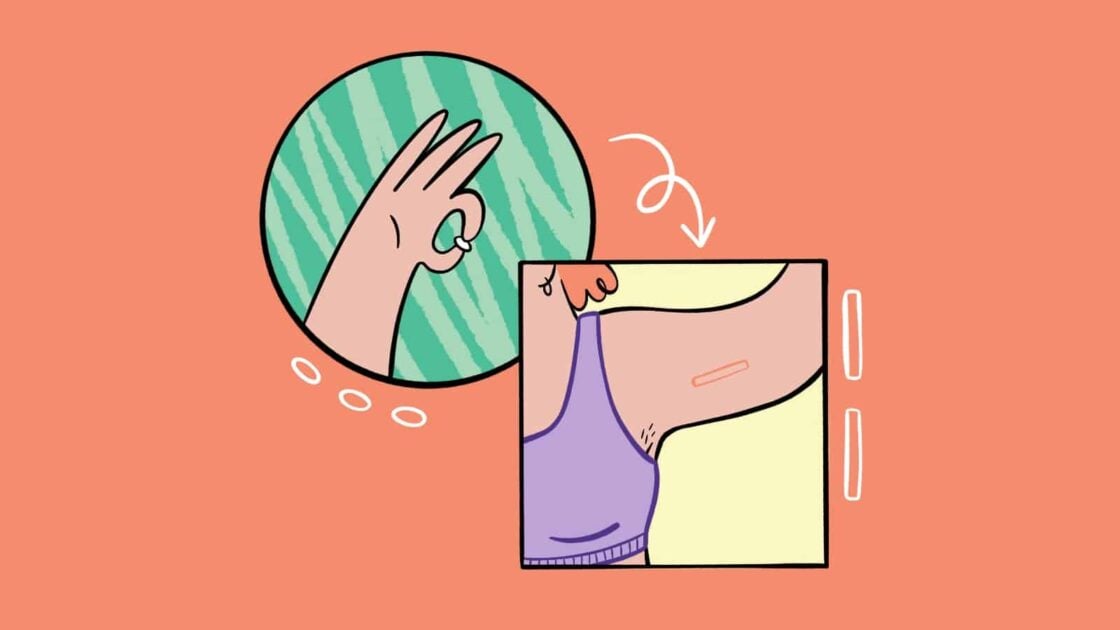
Having decided the pill wasn’t for me, I promptly searched the Internet for viable alternatives. I latched onto the bar. Quick and easy insertion into the upper arm, barely invasive surgery, potential side effects including stopped periods – as far as I could tell, there were no more insidious downsides to this than the pill had. More than that, once inserted, the bar remains functional for THREE YEARS before it needs to be replaced. I stopped taking the pill and placed a GP appointment with no hesitation; I have never looked back.
I will admit that the first few months following the insertion were a rough ride: I was a hormonal, bleeding mess. I was emotional, I was exhausted; I was almost constantly on my period, all while tackling the Christmas exam season – it was not fun.
However, like the storm before the calm, the New Year brought with it the disappearance of my period. It felt like I’d achieved Nirvana. No periods! What every teenage girl dreams of when she’s curled up on her bed clutching a hot water bottle to her stomach and weeping like there’s no tomorrow.
This bliss more or less continued (with the odd spate of light bleeding) for 4 years, after which my period made a comeback. I guess my biggest complaint with the bar is this inconsistency – my period schedule does sometimes decide to shake it up a bit, shifting a week early or a week later, just to keep me on my toes – but for me, the stress relieved by not having to think about the pill every single day is 100% worth it.
No one size fits all with contraception
I need to emphasise that my experiences with specific contraceptives are not universal – the pill does the job for so many people, whilst the bar does not suit some for various reasons (including squeamishness over being able to feel the thing through your skin).
Discontent with sex education, however, is something I have shared and dissected with friends, acquaintances and strangers alike in conversations over the last five years. Too little too late might sum up the general experience. My memory of sex ed. through the pubescent hormonal haze is admittedly not perfect, but I know for a fact that several of my cohorts were already sexually active by the time our sex and consent talks rocked up.
My school taught me the bare minimum, a means to see me through the early experimental years without incurring an unwanted teenage pregnancy. But most women and people with wombs – regardless of where they fall on the spectrums of gender and sexuality – can and do have periods (and sex) for the majority of their adult life. We need and deserve an education in sexual health that reflects that.
This piece is part of ‘Under the Sheets‘, the National Action Panel’s Voices campaign to raise awareness of the importance of unbiased fact-based inclusive sex education for all young people. Access more information and supports for sexual health.
Illustrations by Ezra Pinkerton.
Feeling overwhelmed and want to talk to someone?
- Get anonymous support 24/7 with our text message support service
- Connect with a trained volunteer who will listen to you, and help you to move forward feeling better
- Whatsapp us now or free-text SPUNOUT to 50808 to begin.
- Find out more about our text message support service
If you are a customer of the 48 or An Post network or cannot get through using the ‘50808’ short code please text HELLO to 086 1800 280 (standard message rates may apply). Some smaller networks do not support short codes like ‘50808’.